Age-related Macular Degeneration
Macular degeneration is the leading cause of irreversible severe visual loss in Caucasians age 50 or older in the United States. It has been estimated that this 2.2% of those older than age 65 have worse than 20/200 vision (legally blind) due to this condition. This page discusses the condition known as age-related macular degeneration, or AMD.
Diagnosis of Age-related Macular Degeneration at Richmond Eye Associates
While the treatment of age-related macular degeneration is generally performed by retinal specialists, all of the doctors at Richmond Eye Associates carefully screen patients for retinal conditions such as age-related macular degeneration during comprehensive eye examinations, as well as during examinations focused on visual problems. Recent studies have validated the benefits of supplementation with certain vitamins in preventing deterioration of vision from age-related macular degeneration. However, whether or not these vitamins are recommended is based on the retinal appearance at the time of the eye examination, rather than on symptoms. Thus, it is important to have the retina checked by qualified doctors such as those of Richmond Eye Associates to determine the risk of age-related macular degeneration and what preventive steps should be taken. In some cases, immediate referral to retinal specialists needs to be made, and this can be greatly facilitated by Richmond Eye.
The following sections further discuss age-related macular degeneration and its symptoms, treatment, and prevention.
Types of Macular Degeneration & Risk factors
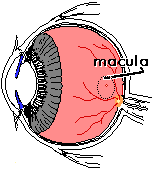 The retina is thin lining of nerve cells which lines the inside of the eye. It receives and processes images, and sends these images to the brain via the optic nerve. The macula is a small, but very important part of the retina capable of perceiving the sharpest of images. It is here where our central vision (what we look directly at), our reading vision, and our color vision are received. Without the macula, we would be legally blind, with only peripheral vision (side vision) to guide us. In the image to the right,
The retina is thin lining of nerve cells which lines the inside of the eye. It receives and processes images, and sends these images to the brain via the optic nerve. The macula is a small, but very important part of the retina capable of perceiving the sharpest of images. It is here where our central vision (what we look directly at), our reading vision, and our color vision are received. Without the macula, we would be legally blind, with only peripheral vision (side vision) to guide us. In the image to the right, 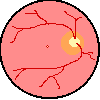 the optic nerve is the yellow circle with blood vessels leaving it. The nerve head is about 1.5 mm in diameter. The vessels are retinal arteries and veins which supply the inner layers of the retina. The center of the macula is the small red and yellow dot, called the "fovea". This is our point of visual fixation (with what we look directly at).
the optic nerve is the yellow circle with blood vessels leaving it. The nerve head is about 1.5 mm in diameter. The vessels are retinal arteries and veins which supply the inner layers of the retina. The center of the macula is the small red and yellow dot, called the "fovea". This is our point of visual fixation (with what we look directly at).
The condition known as "age-related macular degeneration" leads to deterioration of the macula, and possible loss of vision. Risk factors for this condition include:
Age-related macular degeneration is broadly grouped into two categories: a "dry" form, and a "wet" form. The next section discusses these differences.
"Dry" Macular Degeneration
This form of macular degeneration consists of a slow deterioration of the retina. Deposits form between the retina and a layer beneath the retina called the "retinal pigment epithelium". These deposits are called "drusen". Drusen may block nutrition from reaching the retina from a highly vascular layer under the retinal pigment epithelium called the "choroid". The choroid nourishes the outer layers of the retina, while the retinal blood circulation supplies the inner layers. Over time, the retina atrophies, or degenerates, over these area of drusen, and a spotty loss of vision occurs. If more and more of these atrophic areas form and merge together, the macula can take on a moth-eaten appearance, with progressive loss of vision. This usually occurs over a period of many years.
There is no known treatment for this form of macular degeneration, but vitamin supplementation may help to slow or prevent vision loss in some cases. Theoretically, it may help to reduce any risk factors one may have (listed above), but it has not been proven that this will help prevent visual loss. If a person with macular degeneration has a well balanced diet, nutritional supplements may not be necessary. If not, a multi-vitamin is usually recommended (see the section on nutrition below).
"Wet" Macular Degeneration
This is a more severe and rapidly progressive form of macular degeneration. In some cases, the "dry" form of macular degeneration will lead to the "wet" form, but in other cases this form occurs without warning. Between the vascular choroid layer under the retina and the retina itself is a dividing membrane called the "retinal pigment epithelium". If a break occurs in the retinal pigment epithelium, it becomes possible that an abnormal blood vessel could grow from the choroid to directly underneath the retina in the macula. Such a break could occur in an area of drusen, especially drusen that have pigmentation and appear diffuse or fuzzy. When a new blood vessel grows under the retina, it is termed "subretinal neovascularization".
Subretinal neovascularization in the macula can be a surgical emergency. If such a blood vessel is treatable, it should be treated as soon as possible after the diagnosis is made. Symptoms of this condition, otherwise known as "wet" macular degeneration, include:
Note: other conditions such as ocular histoplasmosis, myopic macular degeneration, and macular degeneration related to angioid streaks and trauma can lead to subretinal neovascularization and symptoms such as those listed above. These conditions are often treated in the same way a age-related macular degeneration if subretinal neovascularization occurs.
When an ophthalmologist examines the retina, abnormal blood vessels growing under the retina can often be seen. Other times, there may be hemorrhage in or under the retina, obscuring the view of the vessel. Swelling of the retina can often be observed as well.
Additional tests, such as OCT (Optical Coherence Tomography), fundus photography, and fluorescein angiography, are usually done as soon as possible to better determine where the new, abnormal blood vessel is and if it can be treated.
A fluorescein angiogram is a test done in the office where a pigmented dye is photographed as it passes through the retinal blood vessels. For this test, the eyes are dilated, and initial color photographs are taken of the retina by the photographer. Then, the fluorescein dye is injected into an arm vein by a physician. This is similar to having blood drawn. Once the dye is in, the needle is removed, and the photographs are taken. The dye reaches the eye in a matter of seconds. Abnormal vessels under the retina and areas of leakage from vessels can be clearly identified using this technique, and it is often done to verify the disorder and plan treatment.
Optical Coherence Tomography is a non-invasive test of the retina where reflections from scanning light beam can be reconstructed using a computer to give detailed cross-sectional views of retinal anatomy. This is also used for diagnosis and to monitor treatment success.
Diagnosis & Treatment of Macular Degeneration
The diagnosis of macular degeneration depends on several factors:
The "Amsler grid" is a small graph-like chart with a central dot. It is useful for testing for distortion of vision. To do the test, the grid is held at normal reading distance (16 inches) with glasses on if needed. With one eye covered, the central dot is looked at. Any missing lines, distorted lines, or other abnormality on the chart is then noted by the patient. The other eye is then tested. This is a way for patients with risk factors for macular degeneration, or with previously treated macular degeneration to monitor their vision for development of "wet" macular degeneration (subretinal neovascularization).
To view or print an Amsler Grid, go the Vision Tests Page.
Treatment of "dry" macular degeneration
Treatment Options for Wet Macular Degeneration
Intravitreal Drug Injections
The use of drugs injected directly into the eye has become increasingly used for virtually all forms of wet macular degeneration as well as many other retinal vascular disorders, including vein occlusions and diabetic retinopathy. The identification of the naturally occurring chemical (VEGF - Vascular Endothelial Growth Factor) that leads to the development of abnormal vessels in macular degeneration was a major breakthrough. Various drugs that block VEGF have been developed, and these are known as "anti-VEGF" drugs.
As of 2011, there are several injected drug therapies that are used to treat exudative AMD (wet macular degeneration). Two therapies are approved by the US FDA for this indication: pegaptanib sodium (Macugen®) and ranibizumab (Lucentis®). Intravitreal bevacizumab (Avastin®) and triamcinolone acetonide (and other injectable corticosteroids) are also widely used off-label for the treatment of exudative AMD.
There has been great excitement with the development of these drug treatments, as many patients not only show a decrease in vision loss, many have improvement in vision. While injection of medication directly into the eye does not sound particularly appealing, it is a safe and almost painless procedure performed countless times by retinal specialists. Many patients require multiple injections to control the disease, and slow release medications are under development.
Photodynamic Therapy
Laser treatment of macular degeneration, especially that involving the sharpest area of the vision, has been frustrating, because the laser treatment itself is damaging. Furthermore, the condition often recurs after treatment. An alternative treatment for the "wet" form of macular degeneration has been FDA approved, called Photodynamic Therapy. The "wet" form of macular degeneration consists of abnormal blood vessels growing under the retina, ultimately leading to distortion in the vision, hemorrhaging, and scarring. If these blood vessels (subretinal neovascular membranes) grow under the most sensitive part of the macula (the fovea), laser treatment of the vessels would also destroy the fovea itself, leading to a loss of central vision. Photodynamic Therapy does not damage the retina overlying abnormal vessels, and offers treatment for an otherwise largely untreatable condition.
With Photodynamic Therapy, the drug Visudyne (verteporfin) is first injected into an arm vein. After a short waiting period, a light of a specific wavelength is shined upon the part of the retina that contains the abnormal blood vessels. This light, which has the brightness of a flashlight and is non-damaging, activates the injected drug to destroy the abnormal blood vessels, where it accumulates. Thus, the subretinal neovascular membrane is destroyed while sparing the overlying retina. The whole procedure takes about 20 minutes, and is painless.
The 1 year results of a study looking at the effectiveness and safety of the procedure are favorable. The group of patients treated by Photodynamic Therapy had a 34% better likelihood of retaining vision than an untreated group of patients with the same disorder. In some cases, the vision improved. The procedure did need to be repeated in many patients over a 1 year period to achieve the desired effects. However, there was very little in the way of adverse side effects, with the most common being sensitivity to light for 1 to 2 days.
Other Surgical Options for macular degeneration include manual removal of abnormal neovascular membranes from under the retina in the operating room. Alternatively, the retina itself can be trans-located away from the abnormal membrane and laid back down on a more healthy area of the eye internally. These techniques are undergoing evaluation in carefully selected patients but have not been met with widespread success.
The Benefits of Nutritional Supplements
It has been found that people with diets deficient in certain "anti-oxidant" vitamins and minerals may be at increased risk for age-related macular degeneration. However, a well-balanced diet with the possible supplementation of a multivitamin will usually prevent such a deficiency. Should extra doses of these vitamins be taken by those at risk for macular degeneration?
The retina is at risk for light induced damage termed "oxidative" damage. This damage could possibly lead to macular degeneration. The retina has relatively high concentrations of anti-oxidant vitamins and minerals. These substances help to prevent this oxidative damage. These vitamins and trace minerals include:
- Vitamin A
- Vitamin E
- Vitamin C
- Zinc
- B-Carotene
- Other carotenoids found in foods such as lutein
- Selenium
Different studies have been done to try to determine if there is any relationship between blood level and dietary intake of these substances with age-related macular degeneration (AMD). Some earlier studies were fairly inconclusive as to the benefits of dietary supplements on reducing vision loss from macular degeneration:
AREDS
The landmark AREDS (Age-Related Disease Study Research Group) results indicate a definite reduction in risk of vision loss from macular degeneration with dietary supplementation of antioxidants and zinc. This protection was only evident in those already at moderate or high risk for the disease at baseline, as determined by the retinal appearance at the time of examination. Those studied with minimal or no evidence of macular degeneration at baseline had such a low rate of vision loss from macular degeneration that no treatment effect could be determined. The antioxidants that were found to be effective were:
- Antioxidants (500mg vitamin C, 400 IU vitamin E, 15 mg beta carotene)
- 80 mg zinc, as zinc oxide, and 2mg copper, as cupric oxide
- Both antioxidants plus zinc together
The antioxidants alone reduced the risk of advanced macular degeneration by 10%, the zinc alone by 14%, and the combination of zinc and antioxidants reduced risk by 21%. For more information on this study, and potential risks of these vitamin supplements, go to AREDS Results: High-Dose Supplementation with Antioxidants and Zinc Found Beneficial for those at High Risk for Age-Related Macular Degeneration.
Please note that many vitamins, especially Vitamins A and E can be stored by the body, and dangerous side effects can occur when high dosages of these are consumed. In many people, supplementation with high amounts of zinc may lead to anemia. One study was terminated because high levels of B-carotene consumption were found to increase the risk of lung cancer in male and female smokers. Thus, vitamin supplementation is not without risk, and one's general physician should be consulted prior to taking vitamin supplements. Finally, the body regulates the absorption of many vitamins and minerals. If the body does not need a particular one of these, it may leave the body undigested.
For more information, go to Nutritional Supplements and the Eye.
Please Note:
These sections are not intended to replace the professional examination and diagnosis by a physician, and they are presented here purely for informational purposes. All possible diagnoses and treatment options are not covered, and the information discussed should not be taken as a recommendation to self-diagnose and self-treat a condition. A misdiagnosed or improperly treated eye condition can result in a permanent loss of vision, or a permanent loss of function of the eye or visual system. In the case of any eye problem, seek medical attention promptly. This can include emergency room treatment, as well as treatment by a medical physician or eyecare provider.




